This page is intended for medical professionals seeking evidence-based, clinical information on infant head shape abnormalities.
If you’re a parent visiting this page, please don’t worry if some of the content here feels technical – you are still very welcome to explore, or visit our blog for more accessible guidance.
Call us now on 07982 706454 or 020 7487 4874


The first step in managing an infant cranial deformity is determining whether the cause is synostotic (craniosynostosis) or non-synostotic (positional).
Characterised by premature closure of one or more cranial sutures, synostotic deformities often result in abnormal head shapes that can be severe or syndromic in nature. These require surgical assessment and potential intervention. Our craniofacial surgeons are highly experienced in diagnosing these cases.
More common and benign in origin, positional deformities arise from pressure on the skull – including intrauterine constraint, torticollis, or supine sleeping position (as recommended to reduce SIDS risk). These typically present as a parallelogram-shaped skull (seen from above), as opposed to the trapezoidal shape seen in craniosynostosis.

Clinical diagnosis is usually sufficient in cases of positional deformity; imaging is rarely required. Refer for specialist assessment if:
For infants under 6 months with mild to moderate deformities:
For infants with moderate to severe plagiocephaly (particularly with skull base asymmetry):
In confirmed cases of synostosis, early surgical correction (often within the first year of life) is indicated to:

Regardless of the individual presentation, early identification and referral (where necessary) are key to optimal outcomes. Please consider referral to our clinic if:
Referrals are accepted from GPs, health visitors, paediatricians, physiotherapists, and osteopaths. We also welcome direct parent inquiries.
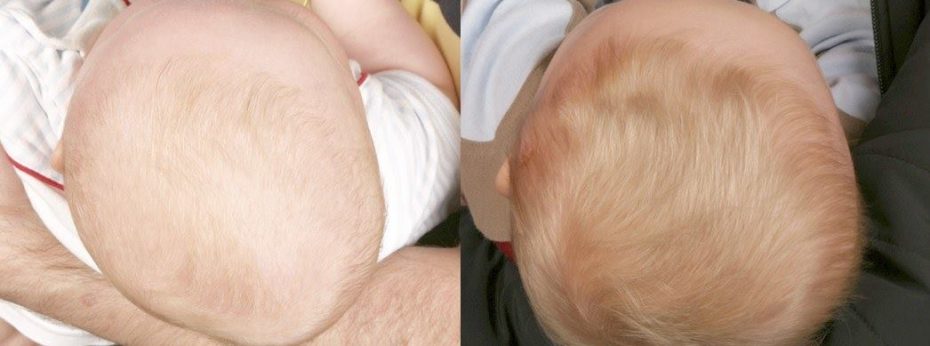
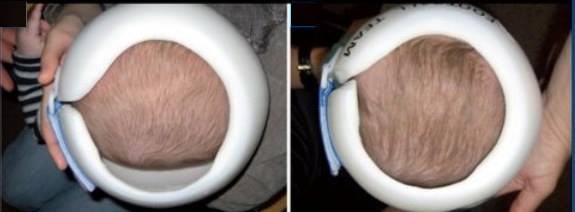
Depending on a variety of factors (including age), helmet therapy may not be right for every child – where it is, early intervention significantly improves the baby’s head shape and overall symmetry.


Led by experienced surgeons specialising in craniofacial deformity, we provide:
Each child is assessed individually. Our treatment plans can be developed collaboratively with parents and referrers, and we ensure regular follow-ups to monitor progress.


Our approach is grounded in published data and long-term follow-ups. Some key findings include:
If you’d like to refer a patient or discuss a case with one of our clinicians, please get in touch.

Founder of Ahead4Babies, Mr Blecher is a highly experienced craniofacial and maxillofacial surgeon treating patients across Europe.

Dr Huppa, a dual-qualified surgeon, specialises in craniofacial deformities and cleft conditions, with extensive international training and expertise.

Dr Stenhouse, a Consultant Maxillofacial Surgeon, excels in managing craniofacial deformities, guiding surgical trainees, and advancing patient care.

Practice manager and plagiocephaly prevention coach Ági Kertész leads a skilled team of administrators and front-line staff coordinating every aspect of the patient experience.
17 Harben Parade, Finchley Rd,
South Hampstead, London NW3 6JP, UK
Yes. It is a non-invasive treatment with a high safety profile. Helmets are custom-made and adjusted regularly. They do not restrict overall head or brain growth.
We welcome self-referrals. We will assess the infant and provide a clear clinical report. With consent, we’re happy to share findings with their GP or paediatrician.
Treatment duration typically ranges from 3 to 6 months, depending on age at start, severity of asymmetry, and compliance. Earlier initiation often results in shorter treatment.
Minor skin redness may be seen, especially during the initial acclimatisation period, but is usually transient. Our surgeons custom-fit each helmet, and are able to adjust the fit precisely for each infant.
Helmet therapy is most effective between 4–12 months, while the skull is still highly malleable. While most helmet providers are unable to offer treatment beyond 14 months due to decreased cranial plasticity, Ahead4Babies’ proprietary, surgeon-designed helmets have shown good results in infants starting as late as 18 months old.
In mild to moderate cases – especially when torticollis is present – physiotherapy and repositioning can lead to good outcomes if started early (ideally before 4 months). More severe or persistent asymmetries may require orthotic support.
Yes. We accept referrals from a wide range of health professionals including GPs, physiotherapists, paediatricians, osteopaths, and health visitors. No formal referral letter is required.
Copyright 2025 Ahead4Babies | All Rights Reserved